Living with the Unknown – Lisa Foster’s Journey with Rare Digestive Disorders
22 April, 2026
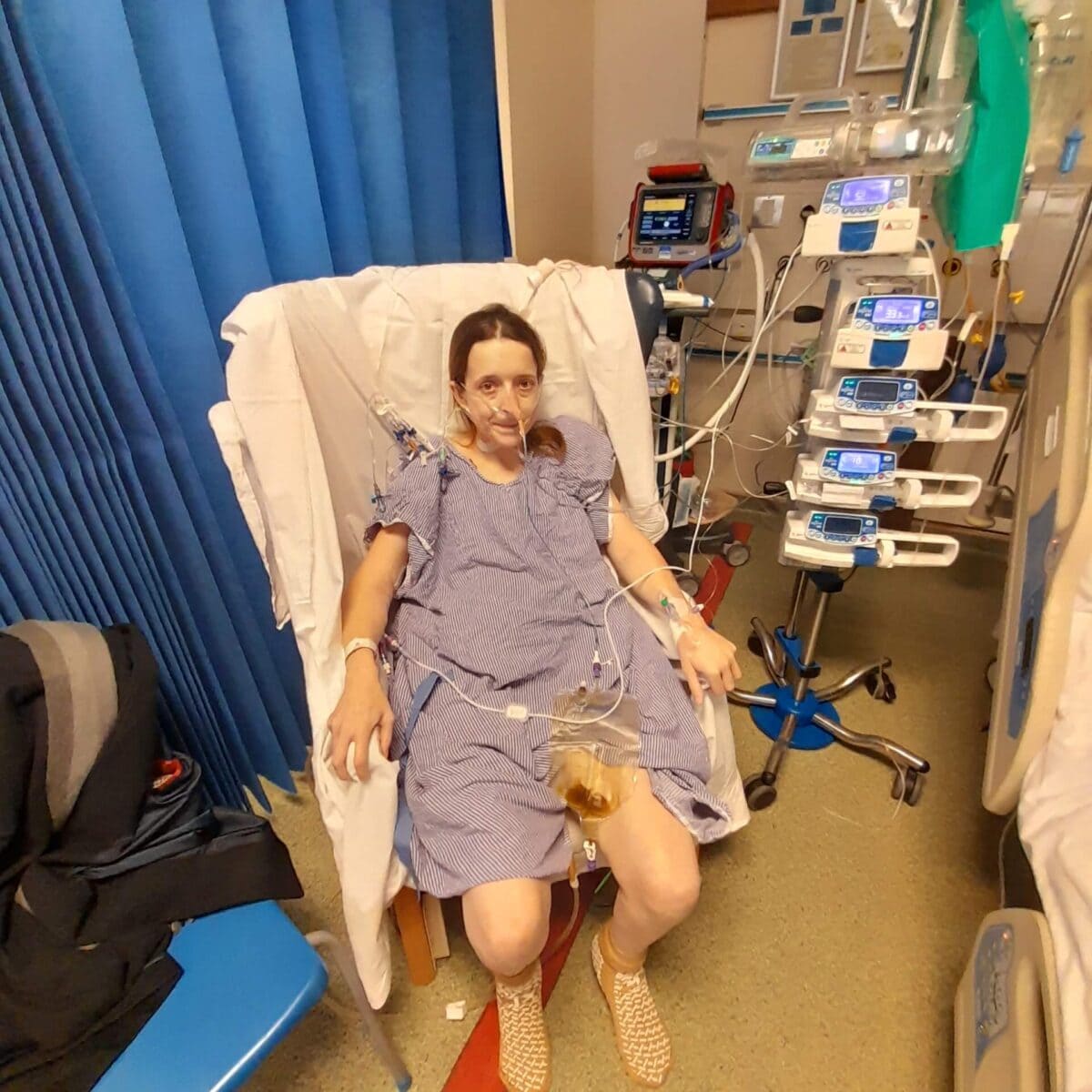
Lisa Foster lives with two rare, incurable, and under-researched conditions. This has meant that her journey to date – as well as what the future holds – have been impossible to predict. Yet one thing that is certain is the new lease of life that Lisa’s stoma has given her.
When Lisa Foster welcomed her son George in 2018, she never imagined that just a few years later she would be facing the most debilitating time of her life – and that George would become a beacon of strength and courage in the way he handled his mother’s illness.
Lisa is living with a permanent ileostomy and navigating the uncertainty of chronic intestinal pseudo-obstruction (CIPO) and mesenteric plexitis. To have one condition on its own is considered very rare – but to have both is extremely unusual. It is estimated that she may be one of only six or seven people in the entire UK who have both. Frustratingly, her consultants admit there is little research to guide them because the conditions are so uncommon.
A Lifetime of Gut Struggles
Lisa’s health struggles began from birth. At times, she would go for long stretches without a bowel movement, sometimes weeks at a time, even as a newborn. For years, doctors dismissed it as “IBS with constipation”, but the true cause was far more complex.
By her late twenties, Lisa developed achalasia, a disorder of the oesophagus that made swallowing difficult and required major surgery. But it was after the birth of George in 2018 that her gut began to fail in far more serious ways. “I once went 24 days without a bowel movement while pregnant,” she recalls. “By the time I had my son, I looked like I was carrying triplets.”
In 2021, her bowels stopped functioning almost entirely. After 49 days without a bowel movement, surgeons performed a subtotal colectomy, reconnecting her small intestine to her rectum. Unfortunately, adhesions later closed that connection, so stomach and intestinal contents had no way to exit and she became very sick. Two weeks later, she underwent emergency surgery to create a permanent ileostomy. “I thought my life was over,” Lisa admits. “But the stoma saved me. Without it, I wouldn’t be here.”
Eight Months in Hospital
Her recovery was anything but straightforward. After surgery, Lisa’s small intestine went into multiple ileus episodes – a form of paralysis in which the bowel refuses to function. Eating or drinking while in ileus can cause serious risks, so the first line of treatment is to be “nil by mouth”, meaning Lisa had to stop all food and drink while her small intestine had a chance to rest. Most patients endure this for two to four days, depending on their circumstances, and are supported with IV fluids in the meantime.
For Lisa, however, things were very different. An unfortunately blunt registrar told her she would be dependent on TPN (total parenteral nutrition) through a central line for the rest of her life, and that she would not live to see 40. “It was devastating,” she says. “But later, I was told by a different intestinal failure specialist that patients can live on TPN for decades. It was a lesson that a prognosis isn’t always fact, and I felt a bit of hope.”
She then had to come to terms with the idea that she would never enjoy food or drink again. Even small sips of water were forbidden. It was hard to imagine, and she struggled with the daily meal service in hospital when others were eating and she had to sit with nothing. Lisa remembers fondly how the nurses helped her through this. “Mealtimes were very hard. I couldn’t eat or drink anything – even a sip of water. But the nurses would sit with me, chat, and keep me company. Their kindness got me through some very dark moments.”
From Hospital to ‘Big Brother House’
One of the hardest parts of Lisa’s long hospital stay was feeling incredibly homesick. She was missing out on everyday family life with her young son George, their two beloved dogs, Milly and Ted, and her wonderful husband, Craig. Visiting was difficult for her family because Lisa was in a specialist hospital, over two hours away from home.
Craig, determined to help her reconnect with home life, came up with a simple but ingenious solution. He installed cameras in their home and garden, then set up a private live stream Lisa could log into from her hospital bed. Suddenly, she could watch George racing around the garden, kicking a football, playing with the dogs, or snuggling down at bedtime with his storybooks. She could hear them and talk to them over a speaker. She could even read George his bedtime stories as Craig sent her screenshots of the book they were reading that night. Lisa jokingly referred to the situation as their own personal “Big Brother House”.
“Of course, it wasn’t the same as being there,” Lisa says, “but it gave me such comfort. I’d log on at night and see George fast asleep, looking so peaceful. It reassured me that at least he was happy and safe.”
That digital connection helped Lisa feel part of family life at a time when she felt incredibly isolated and alone in hospital. It became a reminder of what she was fighting for, and of Craig’s unwavering creativity and love in keeping their family close despite the distance.
The Joy of Eating Again
After more than a year on TPN, Lisa treated herself to “one sip of water” at her husband’s birthday dinner. When she realised her body coped, she checked with her Intestinal Failure Care Team, who advised her to cautiously begin sipping water, then clear fluids like tea and Bovril, and finally soft foods. To everyone’s surprise and delight, her digestion started to work again and by Christmas 2024, she managed to enjoy a festive dinner with her family. “I sometimes cried during those first meals,” she admits. “I never thought I’d taste mashed potato or sit at the table with my son enjoying a meal together again. The feeling of relief and joy was overwhelming.”
Today, Lisa eats a modified diet, avoiding foods that can block her stoma, but enjoys a relatively normal life. She requires regular B12 injections and iron infusions but has regained her strength and her weight mainly through food and drink – something most of us take completely for granted.
George’s Bravery
Lisa and her husband chose never to hide the truth of her condition from their son. Instead, they used humour and creativity to help him understand and cope. Together, they gave her medical devices playful names: her stoma is affectionately called Petunia. She recalls, “Past central lines were Perry the PICC line, Terry for TPN, and Peter for the Hickman line – named after the famous motorcycle racer, since my husband is mad about motorsports. And let’s not forget Nigel the NG tube, who helped me during my long admission.” George, meanwhile, calls her stoma his mum’s “belly bum” – surely the most adorable name for a stoma yet.
George, now seven, has grown up with these realities and has always shown extraordinary empathy and understanding. “I was bursting with pride,” Lisa recalls. “When another child once called me disgusting because of my stoma, George looked them straight in the eye and said: ‘My mummy isn’t disgusting. She’s beautiful inside and out!’ Hearing that from him melted my heart. He’s only little, but he’s already wiser and kinder than most adults.”
Because of how well he has coped, Lisa nominated George for a BBC Make a Difference bravery award last year, recognising the resilience he has shown throughout her illness. He was named a runner-up, and celebrated with a special day out on bumper cars at Weston-Super-Mare pier. “He’s coped with more than most adults,” Lisa says proudly. “He deserved that recognition.”
Craig, too, has been Lisa’s anchor, stepping away from his career to care for her and George full-time, often holding the family together through housing crises, financial strain, medical emergencies, and, sadly, the untimely deaths of their beloved dogs, Milly and Ted. “If I could nominate him too, I would,” Lisa says. “We’ve been through so much as a family.”
Facing the Future
Lisa first reached out to Colostomy UK through Instagram, hoping to raise awareness about rare, incurable diseases such as hers and the many different types of stomas. “Some people think stomas are just about colostomy bags,” she explains. “But each type comes with its own challenges and benefits. I want people to understand it’s not the end of life – it’s the reason I’m still alive.”
She is honest about the difficulties like skin soreness, leaks, fatigue, but also about her gratitude. “I don’t love my stoma, but I accept it. It gave me a second chance. And I’ve learned that life isn’t about waiting for the storm to pass – it’s about learning to dance in the rain.”
Doctors have warned Lisa that her rare conditions may cause further intestinal failure in time, potentially requiring TPN again or even a multi-organ transplant. It is a frightening prospect, but she chooses to focus on the present. “No one knows when their time is up,” she says. “I just happen to live with a bit more uncertainty.”
For Lisa, living with a stoma is not the end of her story, but the beginning of a new chapter. “It hasn’t always been easy,” she reflects, “but it’s given me a strength I never knew I had. My stoma doesn’t define me – it reminds me that I’m a survivor.”
She knows the journey is never all sunshine and rainbows. But she wants others to know they are never alone. “You are not broken,” she says. “You are stronger than your scars, braver than you realise, and you never have to face this journey alone.”







